Mental health practices are growing rapidly across the United States, but managing the financial side of care remains complex. From coding nuances to payer-specific rules, billing for mental health services requires precision, compliance, and a deep understanding of insurance systems. When done right, it improves cash flow, reduces denials, and allows providers to focus more on patient care rather than paperwork.
Key Highlights
• Accurate coding ensures proper reimbursement and fewer claim rejections
• Timely documentation supports medical necessity and audit readiness
• Insurance verification reduces unexpected denials
• Streamlined workflows lead to faster payments
• Outsourcing can improve efficiency and reduce administrative burden
Understanding Billing for Mental Health Services
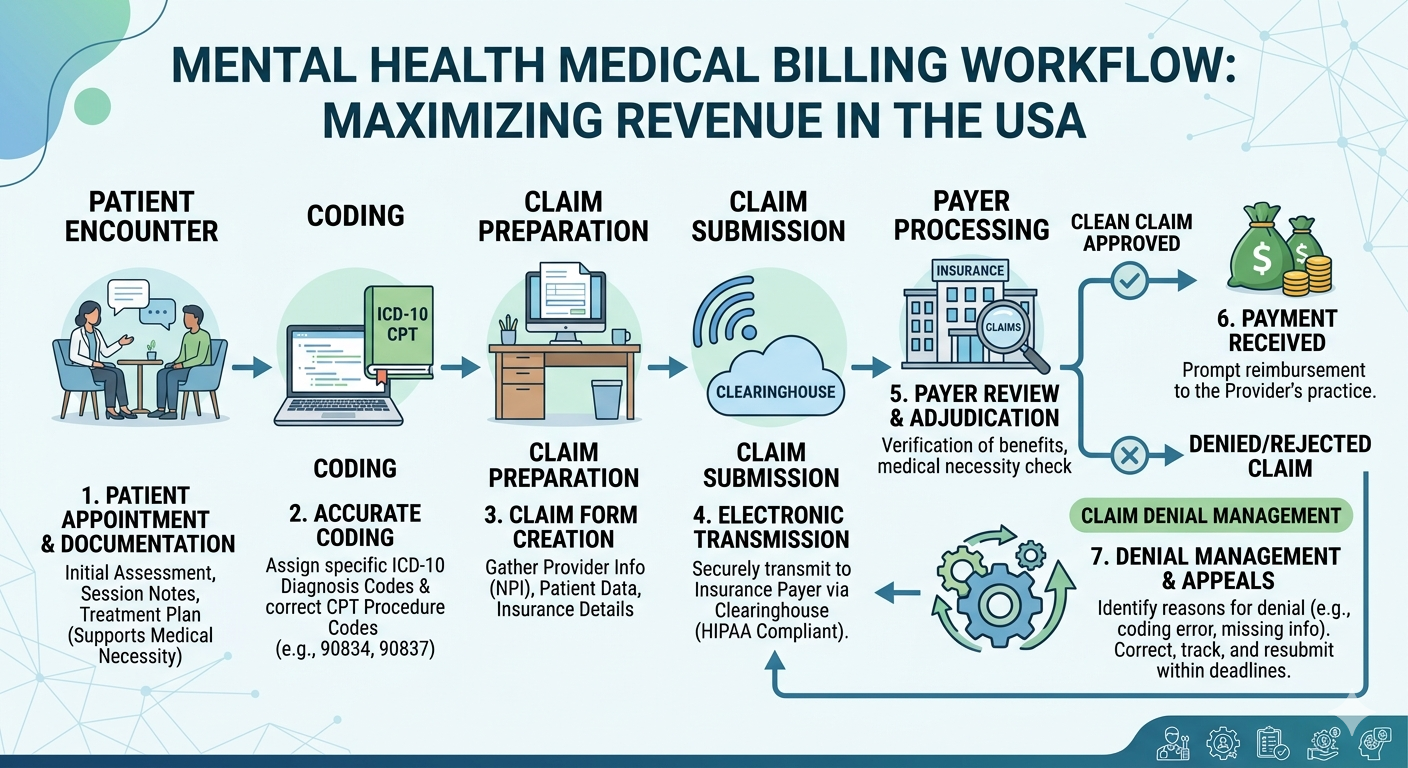
Billing for mental health services involves submitting claims for therapy sessions, psychiatric evaluations, and other behavioral health treatments. Unlike general medical billing, this area includes unique CPT codes, time-based billing structures, and strict documentation requirements.
Providers must navigate payer policies, pre-authorizations, and evolving compliance standards. Whether you are handling billing for mental health providers independently or using professional support, accuracy is critical at every step.
Why Mental Health Billing is Complex
Mental health billing differs from traditional healthcare billing due to several factors:
Time-Based Coding
Many therapy services are billed based on session duration, making precise time tracking essential.
Frequent Policy Changes
Insurance guidelines, especially for billing Medicare for mental health services, change regularly.
Authorization Requirements
Many insurers require prior authorization before treatment begins.
Detailed Documentation
Clinical notes must clearly justify the services provided and demonstrate medical necessity.
These challenges make mental health medical billing one of the most detail-oriented areas in healthcare revenue management.
Core Components of Mental Health Billing
To succeed in billing for mental health therapists and clinics, the following elements must be managed effectively:
1. Insurance Verification
Before treatment begins, verifying coverage ensures that services are eligible for reimbursement.
2. Accurate Coding
Coding and billing for mental health services requires selecting the correct CPT and ICD codes that align with diagnosis and treatment.
3. Claim Submission
Clean claims reduce rejection rates and speed up reimbursements.
4. Payment Posting
Tracking payments ensures that reimbursements match expected amounts.
5. Denial Management
Resolving denied claims quickly prevents revenue loss.
Common Challenges in Mental Health Billing
Even experienced providers face obstacles when handling billing mental health processes:
High Denial Rates
Incorrect coding or missing documentation often leads to claim denials.
Underpayments
Without proper review, practices may receive less than what they are owed.
Administrative Burden
Managing billing internally takes time away from patient care.
Compliance Risks
Failure to follow regulations can result in audits or penalties.
To overcome these issues, many providers adopt mental health billing solutions that streamline operations and improve accuracy.
The Role of Technology in Mental Health Billing
Modern mental health billing services rely heavily on technology to enhance efficiency. Electronic Health Records (EHR) systems, billing software, and automation tools help practices:
• Reduce manual errors
• Track claims in real time
• Improve reporting and analytics
• Ensure compliance with payer requirements
These tools are essential for both small practices and large behavioral health organizations.
Benefits of Outsourcing Mental Health Billing
Outsourcing mental health billing has become a popular strategy among providers seeking to improve revenue cycle performance. Instead of managing billing in-house, practices partner with specialized teams that handle the entire process.
Improved Accuracy
Experienced professionals reduce coding errors and claim rejections.
Faster Reimbursements
Efficient workflows lead to quicker claim processing.
Cost Savings
Working with a cheap outsource mental health billing company can reduce overhead costs compared to maintaining an in-house team.
Focus on Patient Care
Providers can dedicate more time to treatment rather than administrative tasks.
Choosing the best outsource mental health billing and coding services ensures that your practice remains financially healthy while maintaining compliance.
Mental Health Billing and Credentialing Services
Credentialing is a critical step in ensuring providers can bill insurance companies. Mental health billing and credentialing services work together to:
• Enroll providers with insurance networks
• Maintain updated credentials
• Ensure compliance with payer requirements
Without proper credentialing, claims may be rejected even if the services are valid. This makes it an essential part of the overall billing process.
Billing for Mental Health Clinics vs Individual Providers
The billing needs of clinics differ from solo practitioners:
Mental Health Clinics
Billing services for mental health clinics often involve managing multiple providers, handling higher claim volumes, and ensuring consistent workflows.
Individual Providers
Billing for mental health providers working independently focuses more on simplified processes and cost-effective solutions.
Both require tailored strategies to optimize revenue and minimize errors.
Medicare and Mental Health Billing
Billing Medicare for mental health services requires strict adherence to federal guidelines. Providers must:
• Use approved CPT and ICD codes
• Follow documentation requirements
• Understand coverage limitations
Medicare policies can differ significantly from private insurers, making expertise essential in this area.
Best Practices for Accurate Mental Health Billing
To improve outcomes in medical billing for mental health, consider the following best practices:
Maintain Detailed Documentation
Clear, accurate records support claims and reduce audit risks.
Stay Updated on Coding Changes
Regular updates ensure compliance with industry standards.
Verify Insurance Before Each Visit
Coverage details can change, so verification is crucial.
Monitor Key Performance Metrics
Track denial rates, reimbursement times, and claim accuracy.
Use Professional Support When Needed
Outsourced billing for mental health can provide expertise and efficiency.
How to Choose the Right Mental Health Billing Partner
Selecting a reliable provider for mental health billing services is a critical decision. Look for:
• Experience in behavioral and mental health billing services
• Strong knowledge of payer requirements
• Transparent pricing models
• Proven track record of reducing denials
A trusted partner can transform your revenue cycle and ensure long-term financial stability.
Future Trends in Mental Health Billing
The landscape of mental health billing continues to evolve. Key trends include:
Telehealth Expansion
Remote therapy sessions require updated billing practices and coding adjustments.
Value-Based Care Models
Reimbursement is increasingly tied to patient outcomes.
Automation and AI Tools
Advanced systems are improving accuracy and efficiency in billing processes.
Staying ahead of these trends is essential for maintaining a competitive edge.
Conclusion
Billing for mental health services is more than just submitting claims; it is a strategic process that directly impacts the financial health of a practice. From accurate coding to efficient denial management, every step plays a vital role in ensuring consistent revenue.
For providers looking to scale operations and reduce administrative stress, professional support can make a significant difference. Companies like 247 Medical Billing Services offer comprehensive support including medical billing services, medical coding services, medical billing and coding services, revenue cycle management services, and credentialing services. These integrated solutions help practices achieve accuracy, compliance, and sustainable growth in an increasingly complex healthcare environment.
Frequently Asked Questions
What is billing for mental health services?
It refers to the process of submitting claims for therapy, counseling, and psychiatric services to insurance providers for reimbursement.
Why is mental health billing more complex than general billing?
It involves time-based coding, detailed documentation, and varying payer requirements, making it more detailed and regulated.
Should I outsource mental health billing?
Outsourcing mental health billing can improve accuracy, reduce administrative workload, and speed up reimbursements.
What are mental health billing solutions?
These are tools and services designed to streamline billing processes, reduce errors, and improve revenue cycle efficiency.
How does credentialing impact mental health billing?
Credentialing ensures that providers are approved by insurance companies, allowing claims to be processed and paid.
What is the benefit of using billing services for mental health clinics?
They help manage high claim volumes, improve accuracy, and ensure consistent revenue flow.