Mental health practices across the United States are experiencing rapid growth, but along with it comes increasing complexity in billing, compliance, and reimbursement. Mental health RCM billing is no longer just an administrative function; it is a strategic driver of financial stability and patient satisfaction.
From insurance verification to denial management, a well-structured revenue cycle ensures that providers can focus on delivering quality care while maintaining consistent cash flow. This guide explains how mental health RCM billing works, its key components, challenges, and how practices can optimize it effectively.
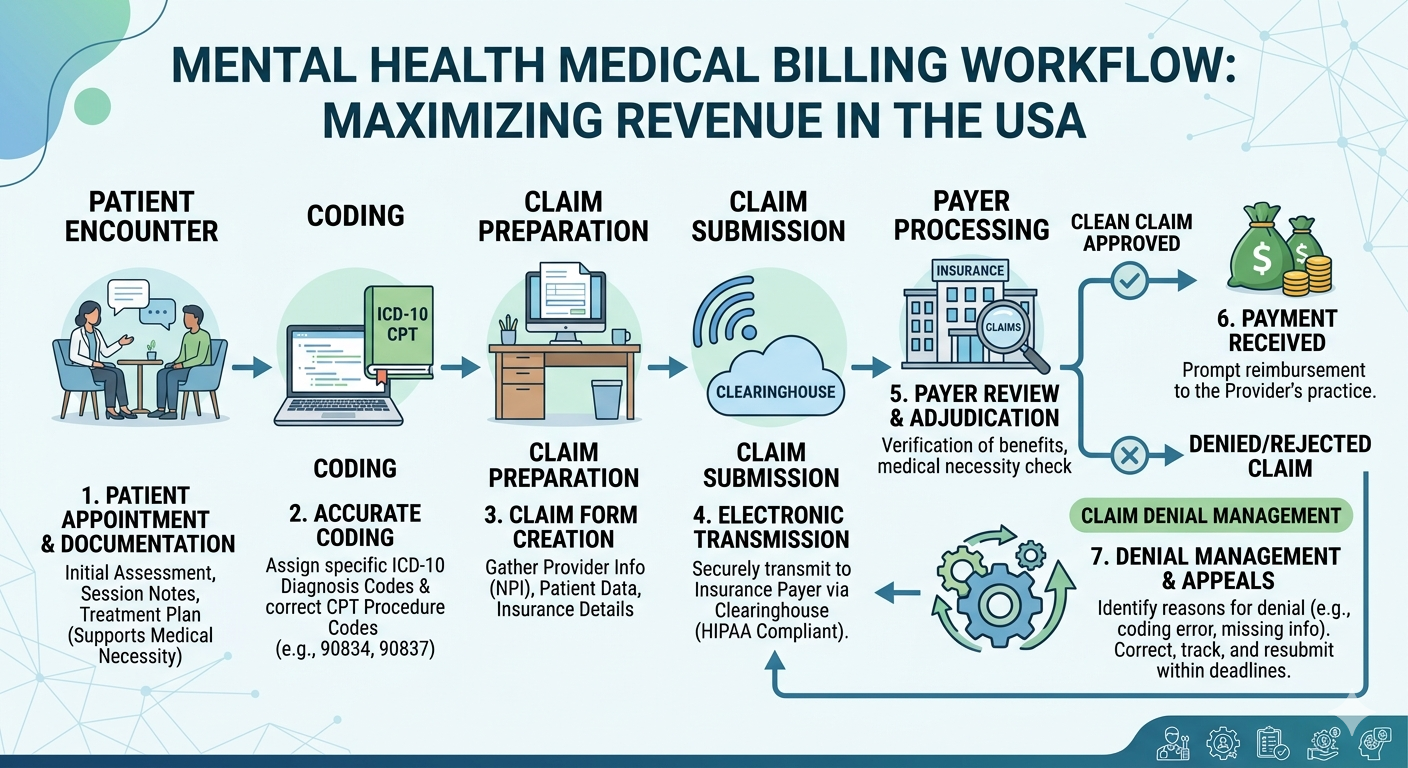
What is Mental Health RCM Billing
Mental health RCM billing refers to the complete financial process involved in managing patient revenue for behavioral health services. It includes every step from patient registration to final payment collection.
Unlike general medical billing, mental health billing involves unique challenges such as session-based billing, time-based CPT codes, prior authorizations, and strict payer guidelines. These complexities make it essential for practices to adopt a specialized approach.
Why Mental Health RCM Billing is Critical
- Ensures accurate and timely reimbursements
- Reduces claim denials and rework
- Improves patient experience with transparent billing
- Supports compliance with payer and regulatory requirements
- Enhances financial visibility and reporting
Without a strong RCM process, even high-performing clinics can struggle with delayed payments and revenue leakage.
Key Components of Mental Health RCM Billing
Patient Registration and Insurance Verification
Capturing accurate patient information and verifying benefits is the foundation. Errors at this stage often lead to claim denials later.
Medical Coding for Behavioral Health
Mental health services require precise coding using CPT and ICD codes. Time-based therapy sessions, telehealth, and group therapy must be coded correctly.
Charge Entry and Claim Submission
Clean claims must be submitted promptly. Practices working with behavioral health billing services connecticut or behavioral health billing services north carolina often focus heavily on improving claim accuracy at this stage.
Payment Posting
Tracking payments from insurance companies and patients helps identify discrepancies and underpayments.
Denial Management and AR Follow-Up
Denied claims must be analyzed, corrected, and resubmitted quickly. This is where outsourcing behavioral health billing ohio or outsourcing community behavioral health billing ohio becomes highly effective.
Patient Billing and Collections
Clear communication with patients regarding their financial responsibility improves collection rates and reduces confusion.
Common Challenges in Mental Health Billing
Complex Payer Rules
Insurance providers have different guidelines for therapy sessions, medication management, and telehealth services.
High Denial Rates
Missing documentation or incorrect coding often leads to rejections.
Authorization Requirements
Many mental health services require pre-authorization, especially in states like those served by behavioral health billing company california or behavioral health billing services california.
Fragmented Systems
Using outdated or disconnected systems creates inefficiencies.
Compliance Risks
Mental health billing must comply with HIPAA and other regulations, making accuracy critical.
Benefits of Outsourcing Mental Health RCM Billing
Many practices are now choosing outsourcing behavioral health billing services florida or outsourcing behavioral health billing texas to streamline operations.
Improved Revenue Cycle Efficiency
Dedicated billing teams ensure faster claim processing and fewer errors.
Access to Expertise
Working with a professional behavioral health billing company connecticut or professional behavioral health billing company new hampshire provides specialized knowledge.
Reduced Administrative Burden
Providers can focus more on patient care instead of paperwork.
Better Denial Management
Experienced teams handle denials effectively, improving recovery rates.
Scalability
Outsourcing allows practices to grow without worrying about billing infrastructure.
State-Specific Billing Considerations
Mental health billing varies across states due to payer policies and regulations.
Practices working with behavioral health billing columbus or behavioral health billing columbus ohio often deal with Medicaid-specific requirements. Similarly, behavioral health billing ohio and top behavioral health billing company ohio services focus on local compliance and payer mix.
In the southern regions, outsourcing behavioral health billing virginia and top behavioral health billing company virginia providers help manage diverse payer requirements. Meanwhile, behavioral health billing company georgia and behavioral health billing services company georgia address regional insurance complexities.
Western states like behavioral health medical billing utah and behavioral health billing services utah require strong telehealth billing expertise. On the East Coast, behavioral health billing services rhode island and professional behavioral health billing company rhode island focus on smaller but highly regulated markets.
For practices in the Northeast, new jersey behavioral health billing and best behavioral health billing services company new jersey provide tailored solutions, while community behavioral health billing services company delaware ensures compliance with community-based care models.
How to Optimize Mental Health RCM Billing
Invest in Specialized Billing Software
Use systems designed for behavioral health workflows.
Ensure Accurate Documentation
Proper clinical documentation supports coding and reduces denials.
Train Staff Regularly
Billing rules change frequently, making ongoing training essential.
Monitor Key Performance Indicators
Track metrics like AR days, denial rates, and collection ratios.
Partner with Experts
Working with best behavioral health billing company south carolina or top behavioral health billing company texas can significantly improve outcomes.
The Role of Technology in Mental Health Billing
Modern RCM systems use automation and analytics to improve efficiency.
- Automated eligibility verification
- AI-driven coding suggestions
- Real-time claim tracking
- Data analytics for financial insights
Technology helps reduce manual errors and speeds up the entire revenue cycle.
Choosing the Right Mental Health Billing Partner
Selecting the right partner is crucial for long-term success.
Look for:
- Experience in behavioral health billing services in california and other regions
- Proven track record in denial reduction
- Transparent reporting and communication
- Compliance expertise
- Scalable solutions
A reliable partner acts as an extension of your practice, ensuring consistent revenue flow.
Future Trends in Mental Health RCM Billing
The future of mental health billing is evolving with:
- Increased adoption of telehealth services
- Value-based care models
- Integration of AI and automation
- Greater focus on patient financial experience
Practices that adapt to these trends will stay ahead in a competitive landscape.
Conclusion
Mental health RCM billing plays a vital role in ensuring financial stability and operational efficiency for behavioral health practices. With increasing complexity in payer requirements and patient expectations, having a streamlined and optimized revenue cycle is no longer optional.
Whether through in-house improvements or outsourcing behavioral health medical billing services provider in florida, practices must adopt a strategic approach to billing. Partnering with experienced professionals ensures fewer errors, faster reimbursements, and better compliance.
At 247 Medical Billing Services, we support healthcare providers with end-to-end solutions including medical billing services, medical coding services, medical billing and coding services, revenue cycle management services, and credentialing services. Our goal is to help practices maximize revenue while focusing on delivering quality patient care.
FAQs on Mental Health RCM Billing
What is mental health RCM billing?
Mental health RCM billing is the process of managing financial transactions for behavioral health services, from patient registration to final payment collection.
Why is mental health billing more complex than general medical billing?
It involves time-based coding, therapy sessions, authorization requirements, and varying payer rules, making it more intricate.
How can outsourcing improve mental health billing?
Outsourcing provides access to experts, reduces errors, improves claim acceptance rates, and ensures faster reimbursements.
What are common reasons for claim denials in mental health billing?
Incorrect coding, missing documentation, lack of authorization, and eligibility issues are the most common causes.
How do I choose the best behavioral health billing company?
Look for experience, transparency, compliance knowledge, and proven results in handling behavioral health billing.
Is mental health billing different in each state?
Yes, payer policies and regulations vary by state, requiring localized expertise for compliance and efficiency.
What role does technology play in RCM billing?
Technology automates processes, reduces errors, improves tracking, and provides insights for better financial management.